技术资料
-
 专家访谈Dr. Judy Mielke and Kate Gardner Funding Research Globally with Dr. Judy Mielke and Kate Gardner of scientifyRESEARCH发布日期: 02/05/2026
专家访谈Dr. Judy Mielke and Kate Gardner Funding Research Globally with Dr. Judy Mielke and Kate Gardner of scientifyRESEARCH发布日期: 02/05/2026 -
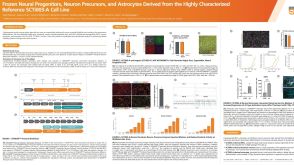 科学海报Frozen Neural Progenitors, Neuron Precursors, and Astrocytes Derived from the Highly Characterized Reference iPSC Line, SCTi003-A
科学海报Frozen Neural Progenitors, Neuron Precursors, and Astrocytes Derived from the Highly Characterized Reference iPSC Line, SCTi003-AConference:
Society for Neuroscience (SfN)
发布日期: 11/12/2025 -
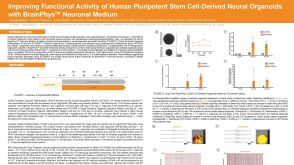 科学海报Improving Functional Activity of Human Pluripotent Stem Cell-Derived Neural Organoids with BrainPhys Neuronal Medium
科学海报Improving Functional Activity of Human Pluripotent Stem Cell-Derived Neural Organoids with BrainPhys Neuronal MediumConference:
Society for Neuroscience (SfN)
发布日期: 11/12/2025 -
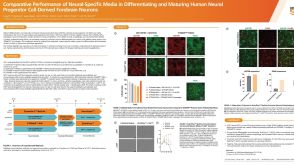 科学海报Comparative Performance of Neural-Specific Media in Differentiating and Maturing Human Neural Progenitor Cell-Derived Forebrain Neurons
科学海报Comparative Performance of Neural-Specific Media in Differentiating and Maturing Human Neural Progenitor Cell-Derived Forebrain NeuronsConference:
Society for Neuroscience (SfN)
发布日期: 11/12/2025 -
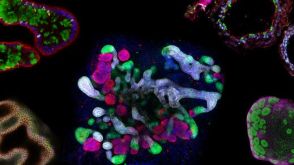 研究综述The Predictive Power of Organoid-Based New Approach Methodologies in Drug Discovery
研究综述The Predictive Power of Organoid-Based New Approach Methodologies in Drug Discovery细胞类型:
上皮细胞,多能干细胞,肠道细胞,肾细胞,胰腺细胞,PSC衍生上皮细胞,PSC衍生肝细胞,呼吸道细胞
发布日期: 10/31/2025

 EasySep™小鼠TIL(CD45)正选试剂盒
EasySep™小鼠TIL(CD45)正选试剂盒












 沪公网安备31010102008431号
沪公网安备31010102008431号